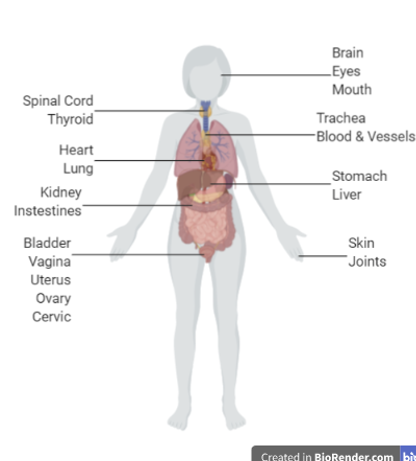
Autoimmune diseases are a family of more than 100 chronic illnesses. It is estimated that they affect more than 23.5 million Americans, which represents about 7% of the population. Autoimmune diseases occur when the immune system malfunctions and starts attacking healthy cells, tissues, and organs. The immune system can target almost any body part, which explains why so many diseases make up the umbrella term “autoimmune diseases” (Figure 1.).
One of the most interesting aspects of autoimmune diseases is their disproportionate effect on women, with women making up more than 85 percent of the patients for some diseases like thyroiditis, scleroderma, lupus, and Sjogren’s syndrome.
Many hypotheses have been formed to attempt to explain these sex differences in autoimmunity, and so far, the focus of many of these theories has centered on the inherent sex differences in immune response that naturally occur due to sex hormones. However, a new hypothesis was recently developed, and it takes a slightly different approach to explain the sex differences in autoimmune diseases. The hypothesis is called the pregnancy compensation hypothesis (PCH).
The components to this hypothesis can be distilled as such:
1. Immune Syste
The female immune system is more robust in both innate and adaptive immune responses.
2. Placenta
a. The placenta and fetus put pressure on the maternal immune system during pregnancy to protect themselves from being attacked by the immune system.
b. The placenta is a highly invasive tissue, and during the process of implantation, it creates an inflammatory response in the mother during the first trimester of pregnancy.
c. In the second and third trimester of pregnancy, the placenta and fetus will shift towards creating an anti-inflammatory response in the mom.
d. The placenta produces estriol which is suggested to have a role in generating immune tolerance during pregnancy and has been found to alleviate several autoimmune diseases.
3. Pregnancy and Lactation
a. During pregnancy and lactation, the mom’s immune system is modulated by the placenta and fetus.
b. The conflict between the mother and fetus is hypothesized to have created selective pressure for the mom to have a flexible immune system at different periods of her life, which does not occur in males.
4. Reproductive hormones
For the first time, humans in industrialized settings are experiencing high levels of sex hormones (e.g. estrogen, testosterone, and progesterone) due to decreases in fertility and increased calorie intake.
5. Sex chromosome dosage
a. X-inactivation — in females, there are two X chromosomes, and one is silenced to ensure that genes are not “doubly” turned on (dosage compensation). However, in humans, many genes on the inactive X chromosome stay on. The genes that “escape” inactivation appear to be random when comparing individuals, tissues, and even cells.
b. Gene dosage on the human sex chromosome is a mechanism by which mom’s immune system evolved to tolerate the invasive placenta.
6. Human Industrialization
a. The absence of exposure to parasites and pathogens in an industrialized setting explains the increase in autoimmunity and cancer — also known as the hygiene hypothesis.
b. Human industrialization has led to fewer pregnancies.
c. Humans have access to more food.
The hypothesis has many moving parts, and many need to be still tested because they have not been proven so far. But overall, this hypothesis attempts to explain the differences in the prevalence of autoimmune diseases between the males and females by pulling in: (1) the ways evolution has shaped male and female immune systems differently; (2) the reduced amount of time pregnant and lactating in industrialized societies; (3) the environmental effects on hormone levels; and (4) gene dosage.
If you are interested in reading more, here are some additional links:
- Sex Differences in Autoimmune Diseases
- Sex Differences in Autoimmune Disease from a Pathological Perspective
- Progress in Autoimmune Diseases Research
- Women and Autoimmune Diseases
Peer edited by Elise Hickman